Medically reviewed by Dr. Brian Paris, D.C on Nov. 6, 2018.
If you’re dealing with a painful sciatica flare-up, you likely have one question on the top of your mind: How long does sciatica last?
I have good news for you if this is the first time you’re experiencing sciatica pain.
Acute episodes generally resolve relatively quickly, usually within a few weeks.
But here’s the rub…
If you don’t identify the root cause of your sciatica pain, there’s a high probability your first episode won’t be your last.
And unfortunately, sciatica flare-up recovery time for subsequent episodes is much longer… and it requires more intervention and a far more comprehensive sciatica treatment plan.
That’s why it’s so important to understand the difference between acute and chronic sciatica, and how you can minimize your chances of further flare-ups down the road.
Table of contents
[1] How long does acute sciatica pain last?
[2] How long does chronic sciatica pain last?
[3] What are the symptoms of sciatica? (And what’s wrong with this question)
[4] The 4 most common sciatica causes
[5] The best sciatica treatment: Muscle Balance Therapy™
How long sciatica pain lasts: acute sciatica

Acute sciatica comes on suddenly and resolves quickly, and usually responds well to self-care measures and home treatments. This type of sciatica lasts on average a few weeks.
(Please note: If your pain is severe and it’s accompanied by muscle weakness and/or loss of bowel or bladder control, you should seek the advice of a medical professional.)
Most mainstream medical doctors will recommend treatment options like over-the-counter painkillers such as NSAIDs.
NSAIDs, or nonsteroidal anti-inflammatory drugs, include popular pain pills like ibuprofen or naproxen.
While these pain medications may help ease your discomfort in the short-term, they come with potentially serious side effects, including an increased risk of heart attack and stroke.
In fact, one recent study found that using ibuprofen — perhaps the most popular OTC NSAID on the market — for as little as a week increased the risk of heart attack by as much as 75 percent. The researchers also found that the risk of having a serious cardiovascular event was greatest within the first month of use.[i]
For short-term pain relief, you’re better off using a combination of natural pain relievers, and alternating between cold therapy and heat therapy.
And most importantly, you need to identify the condition that caused the acute episode in the first place… I cover that more later in this article.
Key takeaway: Acute sciatica comes on suddenly and resolves quickly, and usually responds well to self-care measures and home treatments.
How long sciatica pain lasts: chronic sciatica
If the root cause of your sciatica isn’t addressed early on, the chances are extremely high that you’ll develop chronic sciatica: recurring flare-ups that last longer and require more extensive treatment.
It’s not a matter of IF you’ll have sciatic nerve pain again, it’s a matter of WHEN.
At that point, your doctor or healthcare provider may prescribe stronger painkillers, take a variety of imaging tests, or refer you for physical therapy.
In extreme cases, the treatment options become even more invasive… maybe steroid injections … and in some cases, surgery may even be recommended.
Now, I’m not a fan of putting your body through the trauma of surgery unless there are no other options.
And when it comes to sciatica, that’s just not the case.
In fact, one study found that the outcomes for people who chose nonsurgical, conservative treatments to relieve sciatica pain were nearly identical to those who underwent surgery at 12 months, and were comparable at three and six months.[ii]
The risk of the surgery itself and potential complications are not the only reasons I don’t support it as a go-to solution to relieve sciatica pain.
While the surgery can help ease the pain, it does not address the underlying issue that caused the sciatica in the first place.
It’s critical to not only treat the pain, but the underlying condition responsible for the pain.
If you don’t, you will likely find that sciatica is a lifelong condition.
And that means a life spent managing chronic pain.
Key takeaway: If you don’t address acute sciatica flare-ups properly early-on, you will most certainly be setting yourself up for recurring flare-ups in the future.
Sciatica symptoms
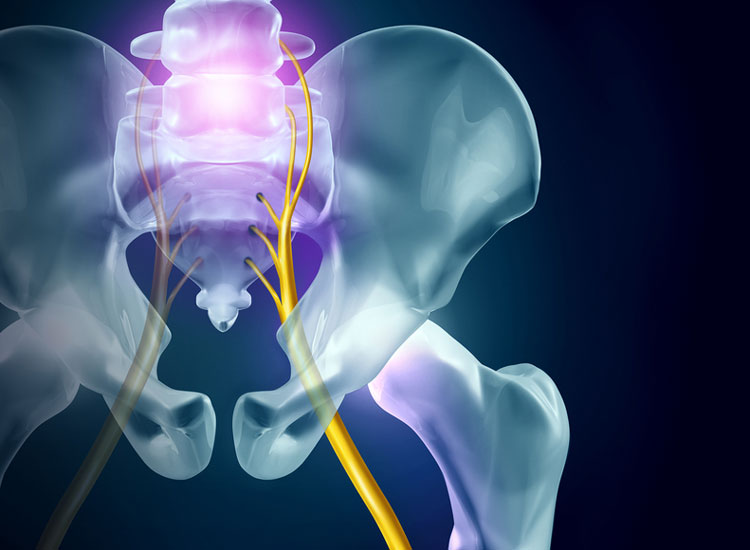
The sciatic nerve is the longest and widest single nerve in your body, running from your lower spine down each leg and ending in each foot.
If you’ve ever known anyone who’s had sciatica pain — or if you’ve been unlucky enough to have experienced sciatica yourself — you may be familiar with the “symptoms.”
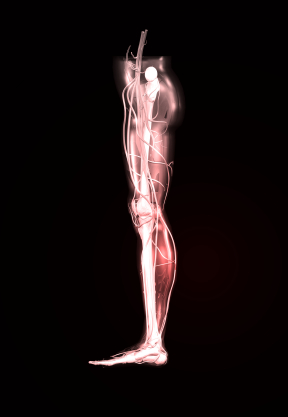
Pain that extends from your lower (lumbar) spine to your rear and down the back of your thigh and/or calf, usually just on one side of the body.
Many people complain of leg pain and have trouble walking.
The pain may be a mild ache, or it may feel like a sharp, burning sensation. For some people, sciatica pain can be downright debilitating.
Some people also have numbness, tingling or muscle weakness.
The exact location of your symptoms will depend where the sciatic nerve is pinched.
But here’s something to keep in mind: Sciatica is not the real cause of that pain. It’s not a diagnosis.
Sciatica refers to the pain, numbness and other symptoms caused by compression or inflammation of the sciatic nerve.
In other words, sciatica is a symptom of an underlying problem — a problem that affects your sciatic nerve.
Key takeaway: Not everyone will experience sciatic nerve pain the same way, but common symptoms include leg pain, muscle weakness, tingling and numbness.
4 most common sciatica causes
Sciatica is almost always caused by one of the following conditions:
1. Piriformis syndrome
The piriformis muscle is a flat, band-like muscle located near the pelvis, sacrum, a lower part of the spinal column, and your gluteus minimus.
It helps your hip rotate and abduct, which is necessary for walking or running.
Piriformis syndrome is a neuromuscular condition that develops when this muscle compresses the sciatic nerve, causing it to become irritated.
2. Herniated discs
If you’ve been told you have a herniated disc, a slipped disc, a prolapsed disc, a bulging disc, a ruptured disc, or even degenerative disc disease, it’s essentially the same thing. There’s no single standard term for this condition.
A bulging disc occurs when the outermost part of one of your spinal discs begins to weaken and the inner soft part starts to press outward, creating an outward bulge.
When the inside material, called the nucleus pulposus, breaks through the disc’s annulus — the tough outer wall — you have a herniation.
If this protrusion touches your sciatic nerve, you have sciatic pain
The location of the bulging disc, and where the sciatic nerve is pinched, will determine where you’ll feel the pain…
3. Spinal stenosis
Spinal stenosis is a condition in which the spinal canal narrows, compressing or “squeezing” the spinal cord and nerves inside.
For some people, spinal stenosis is congenital, caused by imperfections in the development of the spine.
Other causes include a herniated disc, osteoporosis, a tumor, or calcification, which is often the result of nutrient imbalances in the diet.
Another often overlooked cause of spinal stenosis is a build-up of fibrin (scar tissue) brought on by the reduction in proteolytic enzymes in the body as we age.
4. Isthmic Spondylolisthesis
Isthmic spondylolisthesis occurs when one of your spinal discs slips out of alignment and on top of the one below it.
This condition develops as a result of a stress fracture to a small piece of bone that connects the two joints on the back of the spine, called the pars interarticularis.
This misalignment can cause the sciatic nerve to become pinched, leading to sciatic pain.
Here’s what I want you to understand…
Each of the four conditions I listed above has an underlying cause, too: muscle imbalances.
In fact, in nearly every case of sciatica, muscle imbalances are the primary cause of the pressure being placed on the sciatic nerve…
Don’t be surprised if you have not heard this from your doctor. In fact, your doctor probably doesn’t know much, if anything, about muscle imbalances.
Doctors are trained to treat symptoms, not the underlying causes of those symptoms.
Key takeaway: The most common causes of sciatica pain are piriformis syndrome, herniated discs, spinal stenosis and isthmic spondylolisthesis. Muscle imbalances are usually at the root of those four conditions.
This treatment option will help eliminate your sciatica pain
It took me years of research to learn the true root cause of most back pain issues (including sciatica).
Addressing muscle imbalances is the most important step you MUST take if your goal is lasting pain relief.
Simply put, a muscle imbalance occurs when one muscle (or group of muscles) works harder than they should, while other muscles don’t work hard enough. This can eventually lead to sciatica nerve pain.
You see, the muscles in your body work in balanced symmetry — much like the wheels of a car.
When the wheels are out of balance, you’ll begin to notice uneven wear on the tires.
The car will start to pull to one side… you’ll get poor gas mileage… and you run the risk of doing permanent, of a complete tire blowout.
The same is true with the muscles in your body.
When some muscles don’t function as they should, the others have to pick up the slack. And that throws them completely out of whack.
And when your muscles are out of balance, they pull your bones and joints out of their normal position — and this places them under constant and uneven stress and strain.
And these muscle imbalances are the hidden cause of nearly every case of back pain you’re experiencing — including the conditions that lead to sciatica pain.
In the video below, I show you how muscle imbalances cause back pain.
(Want to fix your muscles imbalances now? Click here to learn about my Lose the Back Pain system)
The key to fixing the root causes of your sciatic pain requires some additional lifestyle changes, which will benefit you in the long run in many ways.
Along with fixing your muscle imbalances, you should choose a diet that includes foods that reduce inflammation in your body.
These lifestyle changes may seem like more work than popping Advil every time you have a flare-up, but they will provide lasting relief from sciatica pain.
Key takeaway: Addressing your muscle imbalances is the most effective way to heal and prevent sciatica.
Final thoughts and key takeaways
The frequency and duration of your sciatica pain depend on how and when you choose to treat it.
But in all cases, you must treat the underlying issue or you will almost certainly face sciatic nerve pain flare-ups in the future.
Key takeaway #1: Sciatica pain is a symptom of larger underlying pain conditions.
Key takeaway #2: Modern mainstream medicine suggests taking NSAIDs, such as Advil, to reduce sciatica pain, however NSAIDs can be dangerous to your health and they only address a symptom, not the cause.
Key takeaway #3: For your sciatica pain to go away, you must identify and correct the muscle imbalances in your body.
Key takeaway #4: The best way to treat muscle imbalances is with Muscle Balance Therapy™, one of the core components of my Lose the Back Pain® System.
To learn more about this breakthrough system and lose your back pain once and for all, click here.
Editor’s note: This article has been reviewed by a member of our medical advisory board. The content provided is for informational purposes only and should not be construed as medical advice. Please consult with your physician if you have any questions about your health.
Read more:
Sciatica exercises to avoid: do this, not that
Sciatica and constipation: what helps soften stools
How exercise alleviates sciatica nerve pain
References:
i Bally, Michelle, et al. “Risk of acute myocardial infarction with NSAIDs in real world use: bayesian meta-analysis of individual patient data,” BMJ 2017;357:j1909
ii Peul, Wilco C. et al. “Surgery versus prolonged conservative treatment for sciatica.” N Engl J Med. 2007 May 31;356(22):2245-56.



Does sciatic pain recur despite of doing exercise etc?
I HAVE had major double surgery which has relieved the constant pain though I still have pain depending on what I am doing
HI Helen,
Thank you so much for your comment. You may wish to consider our Book the 7 Day Back Pain Cure. The book discusses back pain and related issues, treatment options to consider, pain relief suggestions, action plans and other helpful information for coping with pain. Please read more about it via the link below
https://losethebackpain.com/products/7-day-back-pain-cure-book
Thank you. Our Best Wishes
Admin (The Healthy Back Institute)
Hi Sarojini,
We have written a book regarding back and sciatic issues that you will find useful to read. It will help you to understand more about the back and to discuss various treatment options.
Please read more about it and get your free copy via the link below.
https://losethebackpain.com/products/7-day-back-pain-cure-book
Thank you
Admin
(The Healthy Back Institute)
Sarojini, sure it can, that is way there are always alternative or additional treatments that you should be ready, willing and able to consider, if such and event does accrue…
That said, we believe that a well balance body it the best defense for future battles of any form of back pain or sciatica, and that is why we try so hard to get people to understand the concept of Muscle Balance Therapy… That is discussed in the book The 7 Day Back Pain Cure
Steve
How long after the pain from my sciatic nerve gets better can I start exercising again such as zumba and other exercises? I have been hurting for about a week but it is easing up and the pain is almost gone
Jessica, It really depends on your tolerance for that activity, that said, the conditions that are in place have are causing you to feel the pain did not just happen overnight, and there should be a concerted effort to address the root causes, in your body, working towards a more neutral balance and stable body will help you tolerate the stress of you day and help you participate at a higher level in any sport or activity you want to take part in… I suggest that you get Jesse’s book The 7 Day Back Pain Cure, that does talk about the causes and treatments for Sciatica. you can find the link to the book on the home page of this site
Steve
I had spinal decompression surgery exactly 5 months ago for a trapped sciatic nerve. The operation was a success in surgical terms but I am still experiencing a lot of pain in my foot (burning and cramping). I am taking gabapentin to help the healing process and to combat the pain but this only dulls the sensation slightly. I do regularly stretching exercises every day. When can I expect things to improve ?
Hi Shaun,
Thank you for your query.
Please take a look at our back pain book which will help you to understand the possible causes of pain and helpful steps for you to consider. You can read more about what is in the book by following the link below.
https://losethebackpain.com/products/7-day-back-pain-cure-book
Thank you
Admin
(The Healthy Back Institute)
Wow!! This sciatica pain came out of the blue with me!! The pain is unberable at times. Hurts so bad,i can not cry. I am 62 years old, white female. does my age cause this ? Do i need to get a shot from my doctor? Pain medicine does not help at all, and i am talking about prescribed medication. I look terrible due to the pain. Hot baths’ do not help either. Makes it worse. Help me please, sir?
Teri,
1. During acute flare-ups, ICE is always best over, heat at least during the first few days.
2.Sciatica its self is a symptom not condition so best to go to the Doctor and get a specific diagnosis as to why you are getting the symptoms you are getting…
3. In the meantime I suggest you get a copy of our Book The 7 Day Back Pain Cure were we talk about all of the different factors that go into having a condition like you do:
https://losethebackpain.com/products/7-day-back-pain-cure-book
Thanks
Steve