Runaway inflammation can stop a beating heart
Inflammation is an important defense mechanism by which our body responds to infection or injury. However, serious problems arise when the inflammatory response gets out of control.
Uncontrolled inflammation directly contributes to diseases such as rheumatoid arthritis, Alzheimer’s disease, multiple sclerosis, and sepsis among many others. But the real killer from runaway inflammation is cardiovascular disease.
Why do we need inflammation anyhow?
Local inflammation in blood vessels activates coagulation, your body’s blood clotting mechanism.
You might remember from health class in school that blood clots are what stop you from bleeding to death when you get a cut.
Here’s how that works in a nutshell. When a blood vessel is injured, specific proteins are released into the blood which makes platelets become “sticky.” In just moments they begin to stick to each other and collagen and adhere to the injured blood vessel wall to form a blood clot.
Two of the main clotting proteins are called thrombin and fibrinogen. Thrombin is “activated” or turned on by the proteins exposed in an injured blood vessel. This activated thrombin breaks down fibrinogen – a soluble liver protein found in the blood – into strands of fibrin, an insoluble protein.
These fibrin strands stick to the exposed and injured blood vessel wall, clumping together to form a web-like mesh of strands. These strands of fibrin trap platelets and sometimes red blood cells to produce a more stable clot, repairing the blood vessel and ending bleeding.
When clotting goes wrong
Although clotting is an important defense mechanism, sometimes it creates new problems. A prime example of this is when blood clots help form atherosclerotic plaques in arteries — which are a major cause of heart attack and stroke.
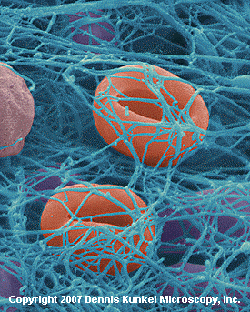
Fibrin traps platelets and red blood cells to form blood clots
Here’s how that happens…
When the inside wall of a blood vessel gets injured and inflamed, our body’s clotting mechanism reacts by weaving fibrin into the wall to strengthen it. This fibrin mesh protects the blood vessel, but also causes it to lose its elasticity. This is the first stage in hardening of the arteries.
Local inflammation from these tears and injuries causes more and more fibrin to be deposited on the artery wall. Fats, cholesterol, calcium and cellular wastes build up on these fibrin meshes and form hardened, calcified atherosclerotic plaques. The arteries become stiffer and less elastic and the lumen (the inner channel of your blood vessel through which blood flows) becomes narrower. This restricts blood and nutrient flow to tissues and raises the blood pressure needed to pump blood through the vessel, leading to even more damage to the blood vessel walls.
Uncontrolled inflammation and clotting cause serious medical problems
Heart attack and stroke
Inflammation hardens arteries, causes atherosclerotic plaques to form and eventually leads to serious medical conditions such as heart attack or stroke.
Blood clots can cause two major problems. First, when a clot blocks a blood vessel, it affects nutrients being delivered to tissues. Second, if the clot breaks free of the blood vessel and begins to travel through the blood, it can become stuck elsewhere in a smaller blood vessel. This blockage, called an embolus, can lead to a heart attack or a stroke if it occurs in the brain.
Deep vein thrombosis (DVT) and pulmonary embolism
If blood flow in the large veins of the legs becomes very slow, the blood may begin to clot and obstruct the veins, known as deep vein thrombosis or DVT. Clotted blood cannot easily pass through the vein and return to the heart. Venous blood clots can also break off or “embolize” and move into the lungs causing a severe, life-threatening medical condition called pulmonary embolism.
An advanced age, birth control pills, inactivity and recent surgeries or injuries all increase risk for DVT. Staying hydrated and moving around regularly helps to increase blood flow and prevent DVT.
Sepsis
Activation of clotting also revs up the inflammatory response. These two defense mechanisms complement each other in their attempt to defend our body against injury and infection.
Once again though, our body runs into serious problems when these responses go out of control. In sepsis, uncontrolled clotting and small blood vessel failure because of a hyper-inflammatory response can lead to multiple organ failure and death.
How to prevent runaway inflammation and clotting

Some drugs can treat abnormal blood clotting but have severe side effects
Conventional medicine likes to throw drugs at most problems, and chronic systemic inflammation, is no different. This inflammatory response triggers blood clotting which leads to dangerous buildups and blockages.
As a result, most drugs used to prevent or treat abnormal blood clotting focus on blocking the clotting process itself or preventing platelets from getting activated.
One class of drugs dissolves meshes of fibrin strands that have already been formed. These “fibrinolytic” drugs are usually administered during the first few hours of a heart attack or stroke to try and re-open a blocked artery and prevent permanent tissue damage from oxygen failure.
But all of these drugs have one very serious side-effect in common: an increased risk of excess bleeding. Fortunately, your body has its own natural solution to the problem of chronic systemic inflammation and abnormal clotting.
Systemic proteolytic enzymes
Proteolytic enzymes, also known as proteases, are commonly known for how they help your body break down food proteins during digestion. But they also travel through your bloodstream where they break down excess proteins like blood clot forming fibrin.
They remove excess fibrin and scar tissue
Systemic proteolytic enzymes breaks down and removes accumulated fibrin, helping clear blood clots and scar tissue from your body. Physicians in Europe and Asia routinely use proteolytic enzymes to remove scar tissue from surgical wounds, fibrotic kidneys and lungs and in other medical conditions.
They improve heart health
When proteolytic enzymes eliminate excess fibrin, it means a reduced risk of clots forming — and a lower risk of heart attack or stroke. More oxygen- and nutrient-rich blood can flow to damaged tissues when blockages are cleared away, which then have a better chance to rebuild and repair themselves as well as remove metabolic waste more efficiently.
They reduce inflammation and fight off infection
Systemic proteolytic enzymes get rid of inflammation by neutralizing pro-inflammatory biochemicals – which is not only good for heart health but also lowers your risk of cancer and Alzheimer’s disease. They help to speed up recovery from sprains, strains, fractures, bruises, contusions and surgery.
Proteolytic enzymes even boost your immune system by helping fight off viral and bacterial infections by seeking out and killing proteins that have viruses attached to them.
Where to get proteolytic enzymes
The good news is your body makes proteolytic enzymes naturally in your pancreas. They are also found in foods such as papaya and pineapple. However, eating these fruits or other sources of proteolytic enzymes within an hour of eating protein will simply divert the use of those enzymes to breaking down your meal instead of helping your body fight inflammation and excess blood clots.
Most people with a chronic pain condition have a corresponding chronic systemic inflammation problem. Inflammation and pain can often both be dramatically reduced simultaneously with an increase in proteolytic enzymes. Consider trying a proteolytic enzyme supplement if you have experienced an injury or have any kind of chronic pain or known inflammatory condition. It can protect your heart and improve your quality of life by reducing pain at the same time.
Click Here Now to…
Try Our Proteolytic Enzyme Supplement for FREE!
References
Levi M, van der Poll T, Büller HR. Bidirectional Relation between Inflammation and Coagulation. Circulation 2004; 109; 2698-2704, DOI: 10.1161/01.CIR.0000131660.51520.9A.
Ridker PM, Cushman M, Stampfer MJ, Tracy RP, Hennekens CH. Inflammation, aspirin, and the risk of cardiovascular disease in apparently healthy men. N Engl J Med. 1997; 336(14):973-9.
Bossù P, Ciaramella A, Salani F, Vanni D, Palladino I, Caltagirone C, Scapigliati G. Interleukin-18, from Neuroinflammation to Alzheimer’s Disease. Curr Pharm Des. 2010 Dec 24.
Robinson T, Smith A, Channer KS. Reversible heart failure: the role of inflammatory activation. Postgrad Med J. 2010 Nov 19.


Hi,
Can we take Heal n soothe when we also take satins (Crestor)? Or should I wait to end the Crestor medication (I have to take it for 2-3 months only) to begin taking HnS? I also take one capsule of Co QH (ubiquinol form), and one Omega3 daily.
Thanks for your answer.
Hi Lale,
Thank you for your question. There is no known interaction between HnS and Crestor but it is suggested that HnS and all medication be taken at least 60 minutes apart. You may wish to discuss further with your doctor.
Thank you
Can this be used with microbleeding in the brain which has recently been diagnosed with tia which resulted in a stroke caused by further bleeding?
Thank you
Hi,
My pharmacist has asked me to take collagen hydrolysate for my inflammation and Osteo arthritis and recommended me the Fishkol brand. The product is manufactured in Japan and is available locally in Malaysia.
I am wondering whether your company has done any research on collagen and it effective in treating arthritis.
Thanks.
Regards,
Philip
We do have a Hydrolyzed collagen product called Super Joint Support, please understand that there are several types of collagen, and the best type of collagen for joint support is Type II, im 90% sure the Fishkol brand uses Type I simple based on the daily dose, of 5 grams, now dont get me wrong Type I collagen has many benefits but it is not optimal for joint health…
https://losethebackpain.com/products/super-joint-support-bottle
Steve
My back problems are long-standing and I get pain from carrying the lightest thing in front of me and also from standing for long periods. One would think that lying in bed would ease the pain, but it makes it even more noticeable. I began taking “Heal-N-Soothe” and had less pain in my back but that made my hip bursitis more noticeable. So I added “Super Joint Support” and day by day the pain eased up to just a minor inconvenience. I ran low on “Heal-N-Soothe” and thought, “I don’t really have much pain anymore, so I’ll just take the “Super Joint Support” and I should be good.” Not so! Within a week, the back pain reared its ugly head and I quickly put in another order. Now I am back on the combination for a couple of weeks. This seems to be the perfect combination for me and I no longer take Hydrocodone to quiet the pain enough to get to sleep. Thank you for your wonderful natural products.
my girl friend woke me up and told me she could not sleep due to throbbing pain in her shoulder. Since I had a bottle of Heal and Soothe with me, I recommended it. within an hour her pain was gone and she was asleep. Next day she keep asking me what was that which I gave her. The whole thing amazed me. Where I used to take heal and soothe for granted, I now am very protective of my bottle of heal and soothe.